Ways to give power to the patients
Get Out-Of-Pocket in your email
Looking to hire the best talent in healthcare? Check out the OOP Talent Collective - where vetted candidates are looking for their next gig. Learn more here or check it out yourself.
 Hire from the Out-Of-Pocket talent collective
Hire from the Out-Of-Pocket talent collectiveHealthcare 101 Crash Course
%2520(1).gif)
Featured Jobs
Finance Associate - Spark Advisors
- Spark Advisors helps seniors enroll in Medicare and understand their benefits by monitoring coverage, figuring out the right benefits, and deal with insurance issues. They're hiring a finance associate.
- firsthand is building technology and services to dramatically change the lives of those with serious mental illness who have fallen through the gaps in the safety net. They are hiring a data engineer to build first of its kind infrastructure to empower their peer-led care team.
- J2 Health brings together best in class data and purpose built software to enable healthcare organizations to optimize provider network performance. They're hiring a data scientist.
Looking for a job in health tech? Check out the other awesome healthcare jobs on the job board + give your preferences to get alerted to new postings.
Powering Patients Up
One big issue with US healthcare is that there are a lot of entities arguing with each other, but patients have almost no say in their decisions. As individuals, we lack agency in the system. We can’t move our data around, we don’t have any good options for care or coverage, we can’t negotiate prices, etc. If I ask how much something will cost, they break my kneecaps and then add that as an ICD code.

Why should we care about giving patients agency?
- If you give enough patients leverage, you can start aggregating that demand to then force the supply side to be more competitive. In industries where there are more options for consumers or when they’re paying directly, you see suppliers and distributors fighting to make things cheaper and easier to access.
- Complexity is a tool used to crush patients, confuse regulators, and make it unclear who’s profiteering. If we can cut through the complexity, we might be able to reduce admin spend, answer these questions clearly/ make changes, and reduce uncertainty in patients’ lives.
- There’s a lot of paternalism in healthcare around what patients should be allowed to do and how much risk they should be allowed to assume themselves. Every patient has a different risk tolerance and is optimizing for different outcomes, but we rely on a top down approach for quality metrics and what acceptable care looks like. No one asks patients what their version of “a good outcome” is, we need to use some dumbass HEDIS measure instead. By giving patients the ability to make their own educated choices they get a healthcare experience they’re happier with, feel more engaged in their care, and we can potentially lower cost.
I’m a believer that we should shift agency to patients, so I wondered if there were areas where this is already happening. Here’s a few places.
Ownership of data
Giving patients ownership of their data so they can take it to other providers, give it to third-party apps they consent to, and potentially make money off their data is something I’ve talked about ad nauseum in the past when discussing data brokers, the return of the personal health record, and interoperability so I won’t rehash those basics here.
But here are some other places patients might can have agency over their own data:
N-of-1 experiments - Patients experiment a lot on themselves when the traditional health system doesn’t seem to have answers. This can be anything from home remedies for dealing with insomnia, testing if people telling you “just don’t be sad” cures depression, to completely new breathing regimens for people dealing with long COVID. More companies and projects are coming up that help patients structure data from their own personal experiments, compare it to other patients like them, and see what works. Companies like Eureka and projects like StudyU are exploring this.

Collaborative health records - Health records should be more collaborative, where patients can add and edit things easily. With the 21st Century Cures Act, patients themselves can now see a whole host of new data - the historical notes that physicians have written about them, insurance coverage data, formulary list, past encounters, etc.
This also provides an opportunity for patients to feel more involved in their health record and potentially take some admin burden off physicians. Here’s a study where patients looked at their ambulatory visit notes and 1/5th found mistakes, 40% of which said they were serious.
Collaborative health records where patients can see everything, make edits, flag certain fields, add their own footnotes, etc. might increase trust between the physician and patient and share the task of documentation between them. Now we can BOTH be at home finishing patient notes until 11 PM 🥲.
Encrypted records - I wonder if the fallout from the overturning of Roe v. Wade is going to make people much more wary about how their health data is used. Let’s be honest, we’re clicking through those terms & conditions faster than a mandatory HIPAA training. But many people rightly started asking questions about how their period apps shared data with a few coming out focusing on local data storage + encryption. Maybe this becomes more attractive for certain people for other areas of health data.

–
Being able to do stuff with your own health data is table stakes for having agency in the healthcare system. By owning your data, you can make sense of your health journey, get guidance on your next steps, and choose who you want to see it. You can’t evaluate different decisions or feel good about making complicated decisions if you aren’t armed with your own data.
It’s a “need to have”, everything else are “nice to haves”.
Giving patients automation
One of the ways that the healthcare system strips patients of agency is by burying them in paperwork, jargon, and making things purposefully hard to navigate. It’s hard to fight back against the system when I’m on the verge of a mental breakdown trying to get a refill of my prescription.
In many cases you have more rights than you think, but these large healthcare entities maliciously comply with them because they know you won’t do anything about it. One of the things that tech does well is not only helping clear things up, but also automating the next steps to take them off your plate.
I’m excited about the prospect of using software to:
- identify people that should be getting some benefit or have a legitimate grievance they should act on
- create and prepare the necessary materials to get what they deserve
- navigate exactly where they should be looking and submitting things
- show them how to move their body to do a celebration dance when they win
A combination of large language models which can generate reports/emails/letters from very little data, robotic process automation that uses computers to replicate human actions like clicking, and advances in machine vision and voice to interpret the world around us are making this possible.
Here are some examples of automation currently at work or could potentially be at work:
Arguing down a bill - DoNotPay is a company that acts as a “robot lawyer”, initially fighting parking tickets using automation. Here’s an example of how it fought a medical bill for a patient by automating the process of asking for an itemized bill, analyzing what was wrong, and then threatening to report the hospital to CMS. This caused them to settle from $1300+ to $150. Lots of companies like Goodbill will also take a look at a bill and see if you were incorrectly billed + dispute it for you and take a % of the savings they get.

Accessing charity care - Ten states have mandates around which patients are eligible for free or discounted care. But this is ONE TRICK HOSPITALS DON’T WANT YOU TO KNOW ABOUT except actually. For example, the Providence hospital system has to give free care for anyone in Washington state below 300% of the federal poverty level (but sent debt collectors to patients anyway because most patients weren’t aware it should be free). Dollar For is a non-profit that helps patients figure out if they’re eligible for charity care, automates some of the process to apply for it, and also has a team to help follow-up on cases.
Superbill automation for claims reimbursement - If you go to a doctor that doesn’t accept your insurance, in many cases, you can still get partially reimbursed. It requires the doctor to create something called a “superbill” which lists the services rendered + info about the doc, and then the patient submits it to the insurance company for reimbursement. The health insurer makes this process so maddeningly difficult that someone wrote an entire story about submitting a superbill to UnitedHealth in the style of a puzzle adventure game as they slowly morphed into the Joker. Some companies do this on your behalf, like Reimbursify, or there’s an actual company called Superbill that either knows SEO or is very literal.
Good faith estimate and the billing dispute process - Because of the No Surprises Act, if you’re not using insurance, you can get an estimate up front from the provider about how much something is going to cost. If it ends up going above $400 from that estimate, you can dispute it within 120 days and get it towards the estimate if you have everything documented. More details on how this works are here, and I assume some companies are or will automate the entire process of requesting the estimate and then disputing it.
A bot listening and responding - I always wish I had a lil’ angel on my shoulder during doctors visits who could tell me when to ask more questions, check if what they’re saying is covered under my insurance, or even be a witness if something went wrong. I always learn things after I get home or try to book a next visit, and I wish I could have done it when I was in the doctor’s office. A company that could be my champion during a visit would be super helpful. The companies like Abridge which record and parse out information from the visit in near real-time might be the closest here.
Voice RPA - I was trying to get a reservation at a restaurant recently and the Google Assistant robot called the restaurant for me to ask about availability and booking the spot. I’m 30 but still get anxious talking to people on the phone, so this was perfect. In healthcare there are so many phone trees, where you’ll inevitably run into a bot yourself. I want to have a bot in my corner to navigate through that bot and the wait times, on some Terminator robot-on-robot violence. Infinitus builds some tools here on the B2B side, but I would love a version for patients to use.

–
Automation can give patients superpowers. Not only will it make it harder for healthcare companies to bury you in bureaucracy as a strategy, but it can potentially aggregate all of those patients together to force those companies to change. Plus, regulation on behalf of patients is only useful if they take advantage of it, which these tools enable.
Now the question is, what’s the business model (since we all know patients will basically never pay out-of-pocket)…
{{interlude 5}}
The transfer of authority
The unfortunate reality is that patients get taken advantage of all the time because they aren’t armed with expertise or authority in the healthcare system, and counterparties know and will take advantage of that. But what if we could give patients more power by arming them with the authority that doctors, lawyers, etc. possess.
Here’s a study that looked at whether landlords responded to fixing housing issues if a pediatrician generated a note to the landlord. About 89% that received the letter actually acted on it. This is a very low effort way to give patients the authority of the doctor in other aspects of their lives that are health related. Apparently there are practical uses of doctor’s notes beyond saying you had a migraine so you can’t come to class when you were actually just hungover.

It can also be your doctor giving you more authority to buy things for their health. For example, letters of medical necessity are essentially doctors giving notes to patients to buy certain things with HSA/FSA dollars or to get insurance to reimburse them. You can see a whole list here, but stuff like air conditioners, certain car modifications, books, etc. can be reimbursed if you get a doctor’s note.

Legal services are another example where the transfer of authority can give patients much more of their time and agency back. Here’s a study from the VA that gave Veterans access to lawyers to help with getting VA benefits, dealing with things like custody/child, credit card debt, etc. Less than 10% of these issues actually required a court appearance - they just required someone who can read legalese without going full narcoleptic + a lawyer that could signal to the counterparty that the patient wouldn’t be bullied. The time spent per veteran here was pretty low and the mental health scores all went up significantly for the veterans.
There are several Medicaid-funded clinics that will incorporate medicolegal services in the clinic as well to help with things like immigration issues, unemployment assistance, fight evictions, etc. NPR writes:
“One woman had been waiting for unemployment assistance since applying in March 2020, and only recently received her first check, says Dale-Ramos. Without legal help along the way, the woman "would have just been like, 'I can't do this anymore,' " Del-Ramos says.
This sort of legal-medical partnership is centered on the notion that doctors can do only so much to keep their patients healthy.
Advocates for such programs cite the example of a child suffering from asthma caused by mold in a dilapidated apartment. While a doctor couldn't force a landlord to clean up the property or allow a tenant to break their lease, a letter from a lawyer might be persuasive, says Dr. Tillman Farley, Salud's chief medical officer.”
Finding low effort ways to get the expertise and authority of someone with a credential can prevent patients from getting taken advantage of + help deal with the other non-medical stressors that manifest as health issues in other ways.
Class actions lawsuits, formal complaints, whistleblowing
The best weapon in a patient’s arsenal is the mfin’ law.
Bounties for whistleblowing, official complaint forms, and class action lawsuits feel like ways the legal system can give patient voices some weight.
For example, in cases of whistleblowing, the person who alerts the government can get 15-25% of the recovered amount. You know the classic saying, “snitches get riches”. When the settlement for a Medicare upcoding scheme is $90M, that’s a fat stack for the whistleblower. Maybe we should make whistleblowing easier as a form of decentralized auditing? There are some companies like Sidesolve that seem to be doing this starting with PPP fraud and looking at other healthcare areas.
I’d be curious if with the new interoperability rules, I could give access to my historical claims/health record data to a third-party to see if it can discover fraud, file a suit on my behalf as a company, and then give me a % of the settlement.
Another way to show the higher powers where to point the auditing gun is to use consumer complaint portals. There is no point complaining directly to the customer service line of a health insurer or hospital because I can only assume they get aroused at your misfortune. But filing a formal complaint with the attorney general of your state (e.g. here’s Pennsylvania) and then letting the insurer know that you did suddenly gets everything moving much quicker. Or here’s ONC’s insanely sketch portal to report if a provider is not giving you the health information you’re mandated access to by law. Most of the complaints filed have been by patients, and now HHS has the authority to go investigate them.
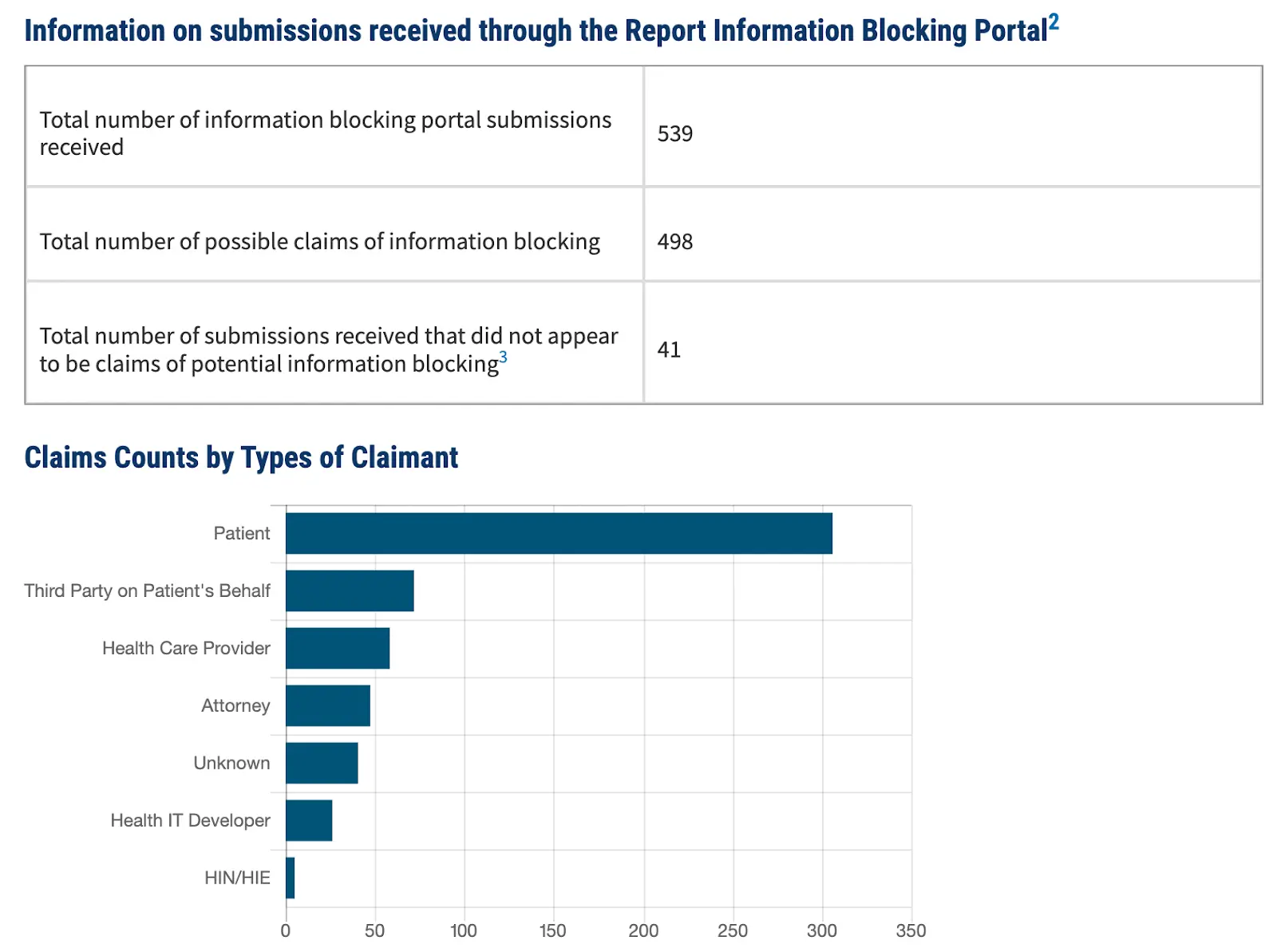
Maybe consumer health apps should have a one click “complain” button embedded in workflows that fills a complaint out and routes it to the right place. Uber basically did this in 2015 by showing wait times within the app if a bill capping number of drivers were instituted, and had an “email now” button to the mayor’s office.
And finally, there’s class action lawsuits. And you know what’s better than suing? Suing with the homies.
I’ve been a part of a few class action lawsuits and the amount I’ve received is probably less than the postage to tell me how much I received. And sure, most of these are lawyers picking specific areas they know they can get a settlement that’s tied to a specific action (e.g. a cybersecurity breach), which probably won’t reshape healthcare.
But it would be cool if we could see more patient-originated class action lawsuits. For example, here’s a lawsuit from 7 individuals against a hospital in Connecticut for their anti-competitive contracting practices. Here’s one where four individuals sued CVS for making them get their HIV meds in a specific location, which posed both privacy and cost issues. I wonder if employees could better hold their employers' feet to the fire with class action lawsuits to make sure they’re acting as fiduciaries in their best interest when it comes to health benefits, especially in the wake of the CAA.
I don’t know if class action lawsuits will completely change things, but it’s a good tool to keep some companies in check. I think people are so angry at healthcare companies they’d hop onto class action suits just on principle alone. I wonder if it’s possible to make that process simpler.
If Swifties not getting concert tickets forced a government investigation into the Ticketmaster monopoly, maybe giving these tools to K-Pop stans will make them look into local hospital monopolies?
The anarchist health system and P2P healthcare
At a certain point, patients and clinicians get fed up with the US healthcare system and its seemingly insane rules. My friends will ask me questions like why their drugs are cheaper paying cash vs. the copay and I just weep softly and open up the job board of a workplace SaaS company just to see what else is out there.
When people really crack, they start looking outside the bounds of the regular healthcare system and into the gray area and more unregulated spaces. This is already happening in certain slices.
- There are gray markets for diabetes test strips where companies will buy boxes from people who are insured and then sell them to people who are uninsured.

- OpenAPS is a community that over the years has essentially “hacked” together a closed-loop artificial pancreas for type 1 diabetics. It’s a Do-It-Yourself process where you load a software script that connects a continuous glucose monitor and insulin pump to automatically give the right dose of insulin. There’s a whole community around improving it and giving tips to others getting started.
- Reddit has an insane number of people that say “doctor here” and then give advice without fear of malpractice but also without the full context usually. Reddit has an r/AskDocs subreddit where the mods verify if you’re a doc and give you “flair” to show that to others.
- Patients are going international for everything from clinical trials for gray area treatments to cheaper medications from pharmacies at the border and procedures like hair transplants.
The reality is that in a lot of cases, patients feel like the rules are actually DETRIMENTAL to their health and are choosing to assume risk themselves. I can see more of this inevitably happening, for better or worse. I would not be surprised if you started seeing more extreme versions of this especially with things like crypto/DAOs as enabling tools to send money with less traceability + provide trust without revealing identity. For example:
- Patients can give their leftover medications directly to other patients who can verify it’s really the medication and they kept it in the correct storage requirements.
- Doctors who aren’t credentialed/licensed in your state and don’t want to reveal their identity can confirm they’re a doctor with on-chain credentialing pseudonymously and give asynchronous or even avatar-based consults. Or imagine you want to get emergency abortion pills mailed via telemedicine in a state with strict abortion laws but no party wants to reveal themselves. Companies like Mayday guide patients through this by showing how to connect mail-order abortion telemedicine (that don’t need a face-to-face visit) with mail-forwarding, for example.
- Any and all do-it-yourself biohacking, like sharing ways with other patients to build your own self-injecting epipens for people that can’t afford the one at the pharmacy.

I’m not condoning this, nor do I think it’s good - it just seems inevitable that this is going to happen as patients get more desperate and the tools become more readily available to make this possible while avoiding consequences. If patients don’t think the rules are in their best interest, they’ll create their own parallel systems which better reflect where they find value and where they want to assume their own risk.
Conclusion
Other industries have transformed because the power balance shifted from suppliers/distributors and into the hands of consumers. Today, the power imbalance in healthcare is still tilted away from consumers, but I’m hopeful that a combination of regulations and software will give more leverage to patients.
Let the revolution begin!
Thinkboi out,
Nikhil aka. "ayyyy guevara"
Twitter: @nikillinit
Other posts: outofpocket.health/posts
Thanks to Elliot Cohen and Sahir Jaggi for reading drafts of this
{{sub-form}}
---
If you’re enjoying the newsletter, do me a solid and shoot this over to a friend or healthcare slack channel and tell them to sign up. The line between unemployment and founder of a startup is traction and whether your parents believe you have a job.
Quick note - Healthcare 101 is back!!!
See All Courses →HEALTHCARE 101 IS BACK BABY!!! In 2 weeks I will teach you about everything you need to know about how US healthcare works. You can see the curriculum online.
It’s hard to figure out how all the pieces work + you don’t know what you don’t know. Archetypes of companies that tend to send employees to this course:
- Services/finance firms that have a healthcare division and want to look smarter to healthcare clients (agencies, dev shops, banking, consulting)
- Health tech companies that have a lot of employees that are not from healthcare
- Large tech/retail companies that are trying to move into healthcare
- International companies trying to understand how the US healthcare market works
- Founders that want to start companies in healthcare
If any of those sound like you, you should sign up. Happy to answer any questions!

Quick Interlude - Data Camp Applications Due Soon!!
See All Courses →Don’t forget…DATA CAMP IS COMING TO YOU THIS JUNE! Applications are due 4/24, but fill it out now before you forget.
More details on the site. It’s all breakouts, a small curated group, and focused on tactical things to bring to work on Monday.
We’re also taking our first sponsors now - so if you want to get in front of data engineers/healthcare data pros, let us know.

Quick Interlude - Data Camp Applications Due Soon!!
See All Courses →Don’t forget…DATA CAMP IS COMING TO YOU THIS JUNE! Applications are due 4/24, but fill it out now before you forget. More details on the site. It’s all breakouts, a small curated group, and focused on tactical things to bring to work on Monday.
We’re also taking our first sponsors now - so if you want to get in front of data engineers/healthcare data pros, let us know.








