The New Price Transparency Laws And Turquoise Health
Get Out-Of-Pocket in your email
Looking to hire the best talent in healthcare? Check out the OOP Talent Collective - where vetted candidates are looking for their next gig. Learn more here or check it out yourself.
 Hire from the Out-Of-Pocket talent collective
Hire from the Out-Of-Pocket talent collectiveHealthcare 101 Crash Course
%2520(1).gif)
Featured Jobs
Finance Associate - Spark Advisors
- Spark Advisors helps seniors enroll in Medicare and understand their benefits by monitoring coverage, figuring out the right benefits, and deal with insurance issues. They're hiring a finance associate.
- firsthand is building technology and services to dramatically change the lives of those with serious mental illness who have fallen through the gaps in the safety net. They are hiring a data engineer to build first of its kind infrastructure to empower their peer-led care team.
- J2 Health brings together best in class data and purpose built software to enable healthcare organizations to optimize provider network performance. They're hiring a data scientist.
Looking for a job in health tech? Check out the other awesome healthcare jobs on the job board + give your preferences to get alerted to new postings.
TL:DR
Turquoise is starting by building the most comprehensive and structured database of negotiated prices between providers and payers, something that’s been secret until now. On top of that, they’re building a set of tools for analyzing price data and using it to power their contracting platform, which makes it simple for anyone to contract with health insurance. If they achieve their goal, they’ll drastically simplify how everyone gets paid and make it easy to shop for cost-effective care. However, they’ll encounter obstacles with enforcement of the regulations that make this data available, competition, and entrenched incumbents who don’t want simple contracts.
Also they built a sandbox with some of the payer data just for OOP readers to play with :).
This is a sponsored post - you can read more about my rules/thoughts on sponsored posts here. If you’re interested in having a sponsored post done, email nikhil@outofpocket.health.
Company Name - Turquoise Health
Turquoise Health is building a database, tools, and collaboration products that live on top of price transparency data. The name comes from the stone Turquoise, which is not transparent; it’s actually very opaque. Like pricing data. No, wait, I got it, is it because Turquoise is the only color left for a healthcare startup since the others used every other shade of blue?
It was founded by Chris Severn and Adam Geitgey and has raised $25M+ from Andreessen Horowitz, Bessemer Venture Partners, Boxgroup, and me! Turquoise was actually my very first healthcare investment when Chris over eagerly filled out my cold pitch Airtable form as soon as I announced it. It’s been very fun to watch their journey over the years and I’m excited I get a chance to talk about them today because I think the problem they’re solving is very meaningful.
[Very cutely, Turquoise is named after the street where Chris met his wife. In which case Hinge Health…🤔]
What pain points do they solve?
Why is it so hard to figure out the prices for anything in healthcare? I’d say there are two core reasons: hospitals don’t want to reveal their prices because it lets them charge more and contracts are so convoluted that it can be hard to actually know the answer.
Because of this reality, a few things end up happening:
- Hospitals and payers end up having to pay a lot to consultants + datasets that approximate the costs of different services to try and figure out what they should be charging or reimbursing. Imagine trying to price your product if you have no idea what your competitors are charging. And you definitely know that averages don’t really make sense since the variance can be as wide as 10x.
- The contracts themselves are stored somewhere “closely guarded” aka. a password protected computer running on Windows Vista, but are a disorganized mess of CSVs, PDFs, and random files that track how much they’re supposed to get paid or pay out. As the contracts themselves get more complicated (e.g. value-based care contracts), the storage and tracking of these contracts becomes even more important.
- Contracting and the management of contracts itself becomes a specialized skill, so if you’re an employer or small hospital that wants to set up your own contracts you basically have to set up your own team or hire the above consultants.
- Patients have no idea how much they’ll end up getting charged and “estimation” tools become useless because they’re based on guesses or proxies instead of the actual contracted rates.

This is rapidly changing thanks to a few different rules that have been passed in the last few years.
- CMS Price Transparency Rules for Hospitals - As of January 2021, hospitals are required by law to publish their contracted prices with every insurer for all items and services in a machine-readable file. This is not an excel file. As a point of reference, a single Mayo Clinic location in Rochester, Minnesotra has over 3.5M distinct rates. My computer fan started blowing just typing that sentence out.
- CMS Price Transparency Rules for Payers - Despite being delayed, this month payer transparency rules go into effect. This includes in-network rates with all the providers, the schedules at which they’re paid, and the amounts they pay for out-of-network providers. IMO, this is where the good shit is, and you can actually see the different fields required by payers in this github schema.

- The No Surprises Act - Starting in January 2022, the only surprises you’ll get are when you look at your 401(k)🥲. Surprise bills will hopefully be a thing of the past (which we talked about here). Instead, if you go out-of-network, your payer and the provider will need to agree on an amount covered.
When you bring all of these together, you have a perfect storm. New pricing data is being unlocked, new processes have to be built (e.g. payer and provider arbitration in the No Surprise Act), and new providers are going at-risk who need to guide patients to more cost effective care.
This is where Turquoise steps in.
What does the company do?
Turquoise is building a new platform for healthcare contracting powered by the price transparency data.
It’s worth talking about Turquoise in phases.
Phase 1 - Healthcare Price Data
Today, Turquoise has built a database of all the available price transparency data that hospitals have put out. In early 2021, there was some comically malicious noncompliance as hospitals remained in denial. Like, instead of saying who the payer was, just saying “Payer 1”, “Payer 2”.
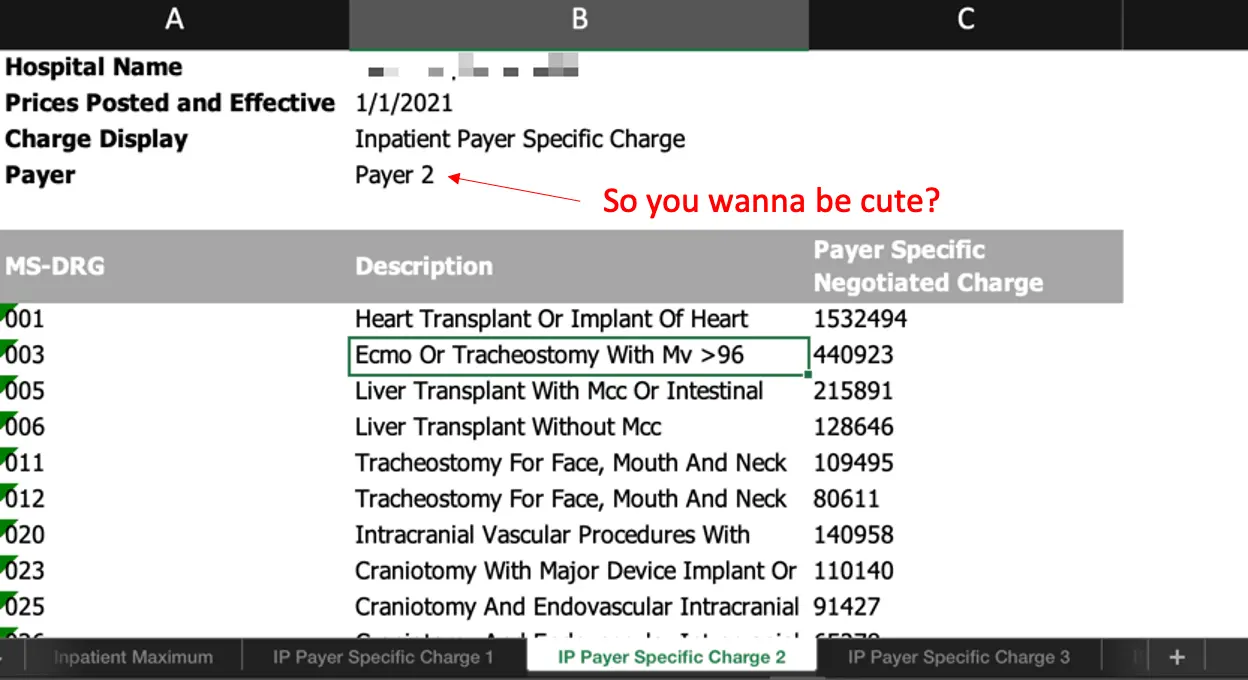
In general, Turquoise retrieves machine-readable files from hospital websites through scraping/digging around, harmonizing that data into a common ontology, running quality checks, and then filling data gaps using machine learning (for example, filling omitted codes based on descriptions if they have confidence).
And now, Turquoise is ingesting the payer data that's being released to a similar common ontology. This data is far more comprehensive than the hospital data as it covers all provider types (not just hospitals) and it’s gigantic. Just for Anthem (I refuse to call them Elevance), each file is 2gb and ~7000+ different files. While they're releasing this sweet, sweet data later this month, they already have a sample dataset available here you can play around with.
But having clean, queryable places for all available price data is just the beginning.
Phase 2 - Contract Negotiation and Management
Once the data is in one place, you can start doing some more interesting stuff. Specifically, Turquoise is building a contract creation and management tool for payers and providers. If price transparency data is being used to help figure out how much a hospital should charge, why not just make the contracting process itself easier?
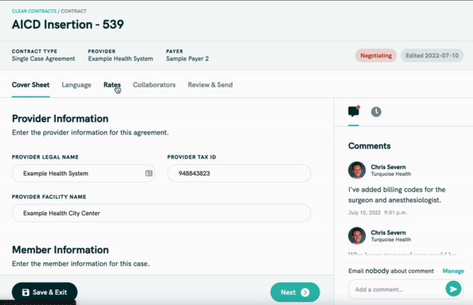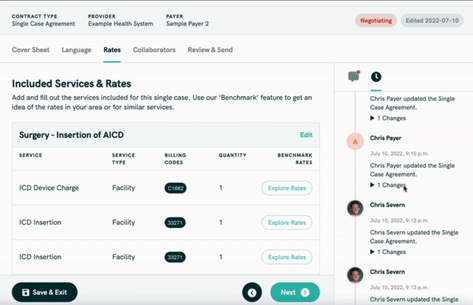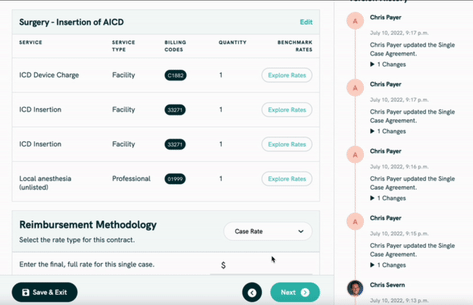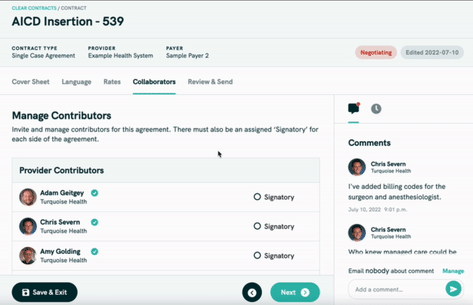
Turquoise has a Clear Contracts product with a few features:
- It uses the price transparency data to show benchmarks within the contract of how other hospitals charge for a given service, which can be sliced by hospital size, geography, payer mix, etc.
- It creates boilerplate contracts that can be easily amended which is useful for both more complex contracts but also one-off on the fly ones that might need to be created if you want to add a provider to your network or negotiate an out-of-network charge.
- Collaboration tools allow all parties to redline, track changes, add comments, etc. within the platform instead of sending Excel sheets and PDFs back and forth labeled “FINAL FINAL 06.22.2022 [2]”.
- It allows payers or providers to combine a bunch of services together and create their own bundles. You wanna throw in a little Diet Coke with your total knee arthroplasty to get the combo for only $5 more? You can set that up here.
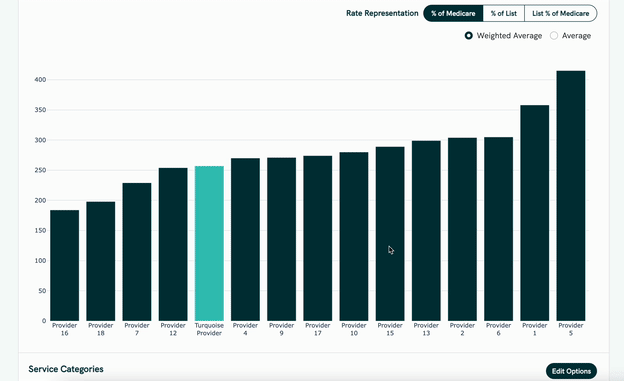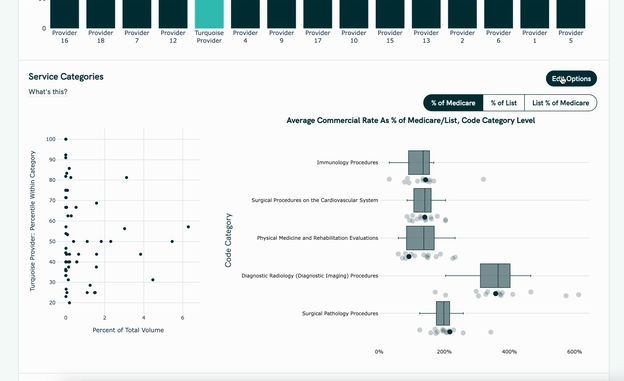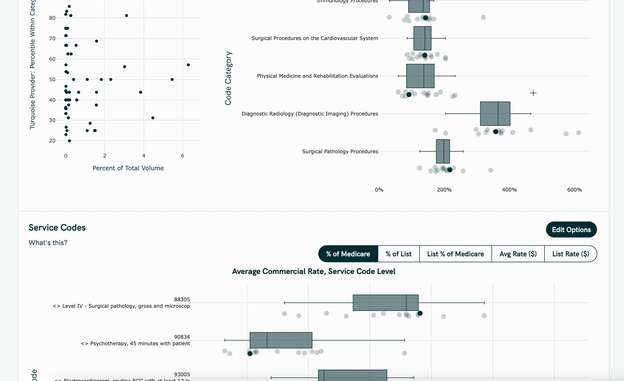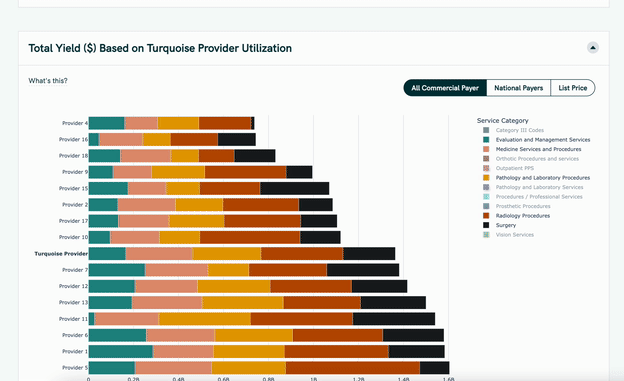
They’re launching with two contract types (and one more on the way).
- Single case agreements, which are one-off contracts for a specific patient, such as when a narrow network payer deals with a member in a sparsely covered region who basically HAVE to go to an out-of-network provider.
- Retrospective batch out-of-network agreements, which are basically reconciling a bunch of out-of-network visits at a given provider. With the No Surprises Act, payers and providers have to come to an agreement or go into arbitration, so it’s much easier to just batch settle at a fair market rate.
- Group health agreements, which are the traditional “negotiate costs and payment schedule for a suite of services” kind of contract. This is coming soon.
What’s the business model and who is the end user?
Let’s once again break this down into phases to understand the use cases.
Phase 1 - Healthcare Price Data
For access to the healthcare pricing data platform, Turquoise charges a licensing fee + recurring annual subscription fee. Straightforward stuff.

There are lots of use cases for this data:
- Patients - Patients can use Turquoise search tools to look up the price of a given procedure in their plan. There are limitations to this tool, so read the FAQ section.
- Providers - If you’re a hospital with a managed care team whose job is to contract with different payers, access to this database + the tools to slice the data will make it much easier to figure out how you should price your services.
- Payers - Payers can design smarter networks by understanding how much hospitals are charging their competitors plus how they charge relative to quality metrics, and then set up incentives for patients to go to the more cost effective sites.
- Pharma/Med Device - When negotiating how much they sell to the hospitals, it’s important to know how much they end up charging the end payer to figure out how much wiggle room they have.
- Care Navigators - Any company whose job is navigating patients to the most cost effective place to get care, images, etc. can pipe this data into their application to help make those decisions. Ribbon Health and Turquoise announced a partnership to combine provider directory data with their prices to make this much easier.
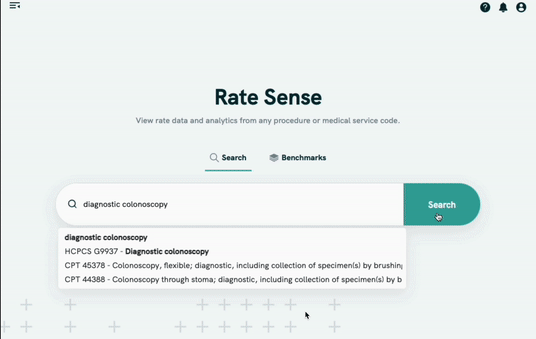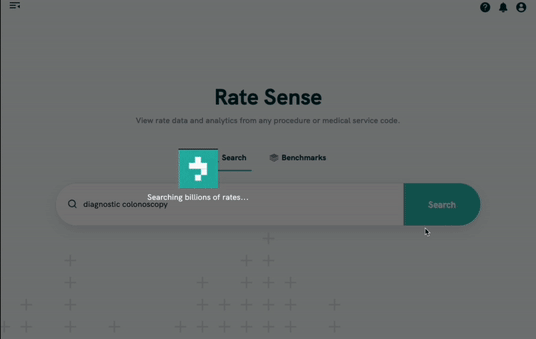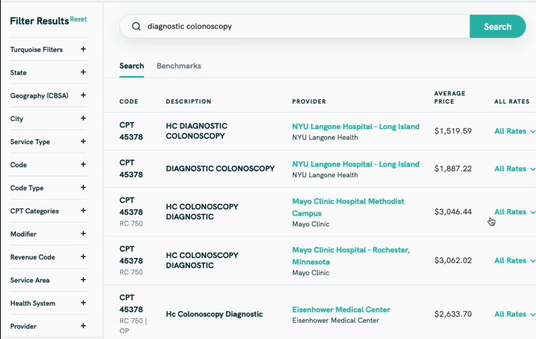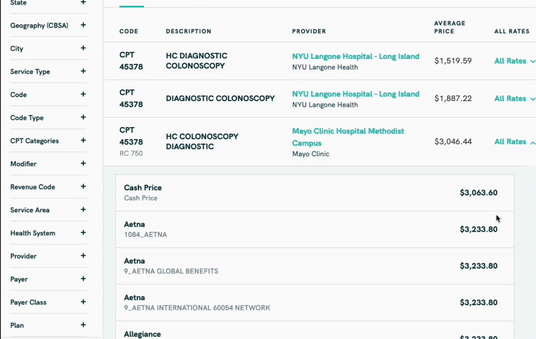
Phase 2 - Contract Creation + Management
Turquoise charges a recurring annual fee based on the number of users and contracts you create and manage on the platform. This is a useful tool for any insurance company or any company that gets reimbursed by insurance.
Some examples of companies that might use this:
- Health insurance carriers - Many new health insurance carriers will “rent” a network of contracts from third-parties so that they don’t have to go to every individual provider in an area and set their own up. However, with the Clear Contracts platform that should be much easier + you can copy rates from similar size payers, since it’s all public.
- Employer - If you’re a self-insured employer (primer here) then you probably rely on a third-party administrator or a health insurance carrier to handle claims, physician network contracting, etc., but lack customization. With Clear Contracts, your benefits team can set up one-off contracts quickly and easily.
- Existing providers - Large providers need to manage tons of different contracts, some of which can be very complex (e.g., buy one get the next one half off). Plus, with the No Surprises Act, they can more easily get paid as an out-of-network provider with some of the Turquoise Contracts.
- New and smaller providers - New startups or practices can get set up quicker by using contract templates and benchmark data. This is actually an opportunity for providers that deliver good care for cheaper (but maybe don’t have the brand name) to show data to payers or employers that they’re a good deal.
Job Openings
Enterprise Customer Success Manager
Senior Data Solutions Engineer, Enterprise
Marketing Manager, Provider and Payer Strategy
Check out their other roles here.
___
Out-Of-Pocket Take
I’m obviously bullish on this company considering my entire retirement plan is now dependent on them succeeding (the original crypto plan has not been going well). If they don’t, I’m going to be living with 3 other roommates for the rest of my life. Please Turquoise, I can’t keep timing my showers like this.
More seriously, I think the price transparency rules represent a paradigm shift in the industry and Turquoise is one of the companies planning to take advantage of this. Here are some of the things I like about Turquoise.
The simplification of contracting - I think complex contracts are one of the roots of all evil in healthcare, along with hospital food. A ton of admin spend is spent managing the contracts and whether payments correctly match them. They’re used to box out new entrants - I’ve been on/heard of many calls where other contracts with competitors will stop a new contract because it trips up something like a most favored nation clause or the dominant player will threaten to pull out of a network if they continue. The industry shouldn’t tolerate that, it’s Scarface style negotiating.
I’m hopeful that Turquoise’s easy to use contracting tool will make it easier for new companies to move from competing because they have leverage via bullying, to competing by actually serving customers. Also, by making contracts easier to understand, they empower smaller companies and remove information asymmetry that usually forces them to take shitty deals.
Simple contracts can make it much easier for new small/medium size businesses to start in healthcare, which would be awesome. It can also meaningfully reduce admin spend by reducing revenue cycle management to fewer steps.

A path to actual healthcare shopping - If there’s one thing old heads in healthcare love doing, it’s talking about how you can’t shop in healthcare. “No one is price shopping in the ambulance” they’ll quip, because they have one joke in their arsenal they took from a viral LinkedIn post.
This feels myopic. It’s true that to date shopping in healthcare has been a failed endeavor, but a big part of that is because you couldn’t shop around without access to the actual pricing data. If you booked a flight, and Kayak told you the ticket range is between $200-$1200 but you’ll find out later, would you consider that an actual shopping experience? The opportunity exists to make a better shopping experience and Turquoise can potentially get us there.
With transparent prices and easier contracting tools, providers now have the ability to actually give price guarantees up front if they feel confident about their quality and the price variance of the given visit. I talked about this years ago. Plus now physicians can actually see the cost of the things they’re asking patients to do. Today, if you ask a provider how much the MRI they ordered is going to cost, they’ll ask what the word “cost” means, as if they’ve never heard it before. But now they’ll be able to shop on behalf of patients for the most cost-effective option, which is especially useful if they’re financially at-risk for the patient’s total cost of care.
Will everything be shoppable? No - you won’t be shopping for the cheapest emergency room when you hit your head against a wall New Year’s Eve 2016 because you somersaulted into it out of excitement and your head starts bleeding (I still went out too). But there are many other areas of healthcare where shopping around is definitely viable, either as a patient or doctor.

The productization of consultants - I think healthcare has the most number of consultants of any industry. In many cases, the consultants pitch their expertise and proprietary data as a way to justify their spend and keep buyers somewhat dependent on them for their services. Managed care consulting - the consulting used to help payers/providers price their services- is an example of this. Turquoise is taking data that’s now public to build tools for buyers of consulting services to either demand more of the consultants they hire or now potentially just do it themselves.
I have a general investing thesis around the productization of healthcare consultants, so if you’re doing something interesting here let me know :).
—
As with any company, there are a lot of things that stand between Turquoise and its goal.
Regulation and enforcement - Turquoise is dependent on the contracted prices actually becoming public and the No Surprises Act actually being enforced. So far compliance from hospitals has been mixed, but a recent increase in fines for non-compliance has led to meaningful compliance by two-thirds of hospitals. The reality is that the original penalty of ~$100K a year wasn’t enough for hospitals to actually care about this, it basically amounted to canning one digital health startup pilot which they were probably going to do anyway. However, the penalties have now been upped to ~$2M a year and the first penalty has officially gone out for a cool milli so CMS is serious about enforcing it.
The payer side has more of the interesting data and the noncompliance fines are supposedly $100 per member per day. At that level, even the health insurers would go bankrupt in a couple of months (and I hope CMS sends a claims denial letter to them along with the penalty, just for irony’s sake). Already in the first two weeks the five largest payers have been mostly compliant.

The fight against transparent contracts and standard fee schedules - Despite making it easy to spin up simple contracts, the reality is that a lot of incumbent healthcare organizations have benefitted from opaque and extremely custom contracts. So, convincing organizations to move to simple contracting is going to be super difficult because frankly it’s not in their interest for a lot of them. The future of the company and therefore the future of my unborn children is betting that eventually they’ll start using software to create and manage these contracts.
But I’m bullish on the smaller companies being first adopters here anyway: small employers who want specific providers in-network for their employees, smaller care delivery startups that want to get contracts setup as quickly as possible. Smaller practices that realize they can get more patients by selling their own bundles and spend less time on admin using simple contracts. New insurers that want to build better networks. Over time, larger enterprises will realize that they’ll save more on admin spend with these simpler contracts.
The commoditization of data + competition - Because this data is slowly becoming more public, eventually it’ll be commoditized. Turquoise has a head start because no one thought the rule was going to be real + they built some nifty tooling to grab, organize, and slice the data. But it likely won’t be their long-term competitive advantage. However, they always knew that, which is why the pricing data is really the fuel that feeds into the other stickier tools like contracting.
This then begs the question: can existing contract management companies or managed care consulting firms that create and manage contracts build the technology to ingest pricing data faster than Turquoise can build the full suite on top of their pricing data?
Nothing…changes - Turquoise could just end up being a tech + services firm that replaces some of the existing consultants, and can build a big business that way. But honestly, I think price transparency will be a failure if it doesn’t actually meaningfully change how they approach pricing and contracts. And it’s possible that the large brand names have so much leverage that they just…don’t care that their prices are transparent and operate business as usual. This is a moment for healthcare companies to lean into transparency as something that can be used to their advantage, but the sluggishness of the industry and their entrenchment might end up with another well-meaning regulation that doesn’t move the needle.
Conclusion
While most people were dismissive, the Turquoise team has believed these price transparency rules are going to be a massive deal since 2019. In 2020 they convinced me of that, too. Sure, it’s still a massive bet that some things are going to go right, but I think if it does go right we might actually see healthcare radically change how it prices.
We’ve talked about the first two phases of the company, but when you’re this close to the transaction between payers and providers, phase 3 gets more interesting. That’s for another day :).
Thinkboi out,
Nikhil aka. “chartreuse health"
Twitter: @nikillinit
Other posts: outofpocket.health/posts
{{sub-form}}
---
If you’re enjoying the newsletter, do me a solid and shoot this over to a friend or healthcare slack channel and tell them to sign up. The line between unemployment and founder of a startup is traction and whether your parents believe you have a job.
But first…DATA CAMP APPLICATIONS CLOSE SOON
See All Courses →If you’re into healthcare data and want to be around other healthcare data nerds, you really should apply to Data Camp ASAP!! The people are saying nice things about it because we do a lot of really awesome workshops to make you better with healthcare data.
Applications are due 4/24, BUT YOU WILL FORGET SO DO IT NOW IT TAKES LIKE 5 MIN IF YOU’RE SMART.
And sponsors…we’re already talking to people and have a limited number of slots. Hit me up if you want to see the packet.
And if you’re REALLY a healthcare data nerd…you’ll want to come to our AI x Risk Adjustment FREEEEE course. You’ll learn at least a thing or two, and probably a lot more. Starts 4/22 (aka…right before data camp applications!)

Quick Interlude - Data Camp Applications Due Soon!!
See All Courses →Don’t forget…DATA CAMP IS COMING TO YOU THIS JUNE! Applications are due 4/24, but fill it out now before you forget.
More details on the site. It’s all breakouts, a small curated group, and focused on tactical things to bring to work on Monday.
We’re also taking our first sponsors now - so if you want to get in front of data engineers/healthcare data pros, let us know.

Quick Interlude - Data Camp Applications Due Soon!!
See All Courses →Don’t forget…DATA CAMP IS COMING TO YOU THIS JUNE! Applications are due 4/24, but fill it out now before you forget. More details on the site. It’s all breakouts, a small curated group, and focused on tactical things to bring to work on Monday.
We’re also taking our first sponsors now - so if you want to get in front of data engineers/healthcare data pros, let us know.








