Patient Communities Should Change
Get Out-Of-Pocket in your email
Looking to hire the best talent in healthcare? Check out the OOP Talent Collective - where vetted candidates are looking for their next gig. Learn more here or check it out yourself.
 Hire from the Out-Of-Pocket talent collective
Hire from the Out-Of-Pocket talent collectiveHealthcare 101 Crash Course
%2520(1).gif)
Featured Jobs
Finance Associate - Spark Advisors
- Spark Advisors helps seniors enroll in Medicare and understand their benefits by monitoring coverage, figuring out the right benefits, and deal with insurance issues. They're hiring a finance associate.
- firsthand is building technology and services to dramatically change the lives of those with serious mental illness who have fallen through the gaps in the safety net. They are hiring a data engineer to build first of its kind infrastructure to empower their peer-led care team.
- J2 Health brings together best in class data and purpose built software to enable healthcare organizations to optimize provider network performance. They're hiring a data scientist.
Looking for a job in health tech? Check out the other awesome healthcare jobs on the job board + give your preferences to get alerted to new postings.
TL:DR the comments section of the internet is good.
I’ve seen a lot of new patient communities pop-up recently. I think it’s the combination of communities being the hot topic in VC land, the idea that communities provide some sort of defensibility for a product, and the fact that everyone is online now and exploring new parts of the internet. But also I think new ways of monetizing are leading to people rethinking what patient communities can look like.
As someone who’s built a few communities and excited by their potential + thinks about what makes them difficult, I thought I’d put some thoughts down.
The value of patient communities
Patient communities are really important for a few reasons.
First of all, patients are already seeking information online about their issues. This can be some combination of the fact that advice from the internet is free, they’re embarrassed about their issues, and they feel the medical system is not hearing what they have to say. However, these communities are almost entirely disconnected from the current healthcare system. At best, moderated communities help patients get answers and support but they exist independent of the care a patient gets with their provider. At worst, there’s no moderation and patients can find themselves suddenly raiding the Capitol. Meeting patients where they are (aka on the internet) can lower the friction for them to get the answers or follow up care they need.
Second, utilizing patient communities well can improve outcomes in a cost-effective way. Cohort-based programs like Omada, Noom, etc. use group chats and group dynamics to keep members engaged and provide positive feedback on hitting goals. This is the cheapest form of patient engagement and support you can get because it’s from other patients. Alcoholics Anonymous is probably the best example of this, and countless studies, meta-studies, and meta-meta-studies have shown this:
Their analysis of 35 studies involving more than 10,000 participants showed that when it came to maintaining sobriety, AA was more effective than psychotherapy or no treatment -- regardless of the age or gender of the study participants, or the country they lived in.
"It absolutely does work…People who are in these groups have 20% to 60% better abstinence than people in other treatments. In no case did they come out worse."
He attributes AA's success to its model of social interaction, in which members provide one another with emotional support as well as practical tips for staying on the wagon. There's a lot of evidence, he said, that surrounding yourself with people who are trying to make the same changes you are is helpful.
Patients that also have a disease can provide much more empathy, social support/pressure to push through difficult parts of treatment, and practical information about living with the disease. This can be anything from understanding side effects of meds or best way to administer them, lifestyle changes that can help with a disease, best ways to navigate the healthcare system and find good physicians, and more. A physician that’s never lived with X disease won’t be able to provide a lot of that information.

And finally, patient communities are good ways to quickly get feedback or user research from a lot of members that might have different experiences with a disease. Most healthcare companies get very little feedback or input from patients directly, and patient communities make it easy to get input from a lot of people with different manifestations of a disease to understand how their lives could be improved. Life sciences companies have utilized this to engage with patients on things like clinical trial design, real-world evidence, etc. But this could potentially extend to things like HCAHPS scores, Star ratings, or anything else that requires some sort of patient feedback.
Patient Communities V1 - Ads, data, life sciences
Online patient communities have been around for a while. In 2001, an article in JAMA where the author talked about the potential of patient communities for rare disease patients as a way to exchange the small amount of information available, provide emotional support, and get explanations in plain terms.
According to an old adage, "Man loves company even if only that of a small burning candle." [NK note: people that wrote old adages were lonely af] The process of exchanging ideas via the Internet can be therapeutic for people with rare diseases. Practical ideas as well as emotional support emerge from Internet discussions among members of rare-disease communities, since by comparing treatment courses, patients may get ideas for their own treatment. The Internet has already helped to create important new communities for patients with rare diseases, the medical community, and the general public. By using the Internet, many more rare-disease communities will be able to share experiences, resources, ideas, coping skills, helpful hints, financial support, and hope.
In 2006, PatientsLikeMe launched its first patient community after the founders’ brother was diagnosed with ALS. On Reddit, different subreddits were popping up dedicated to different diseases. Facebook groups for health conditions emerged as well.
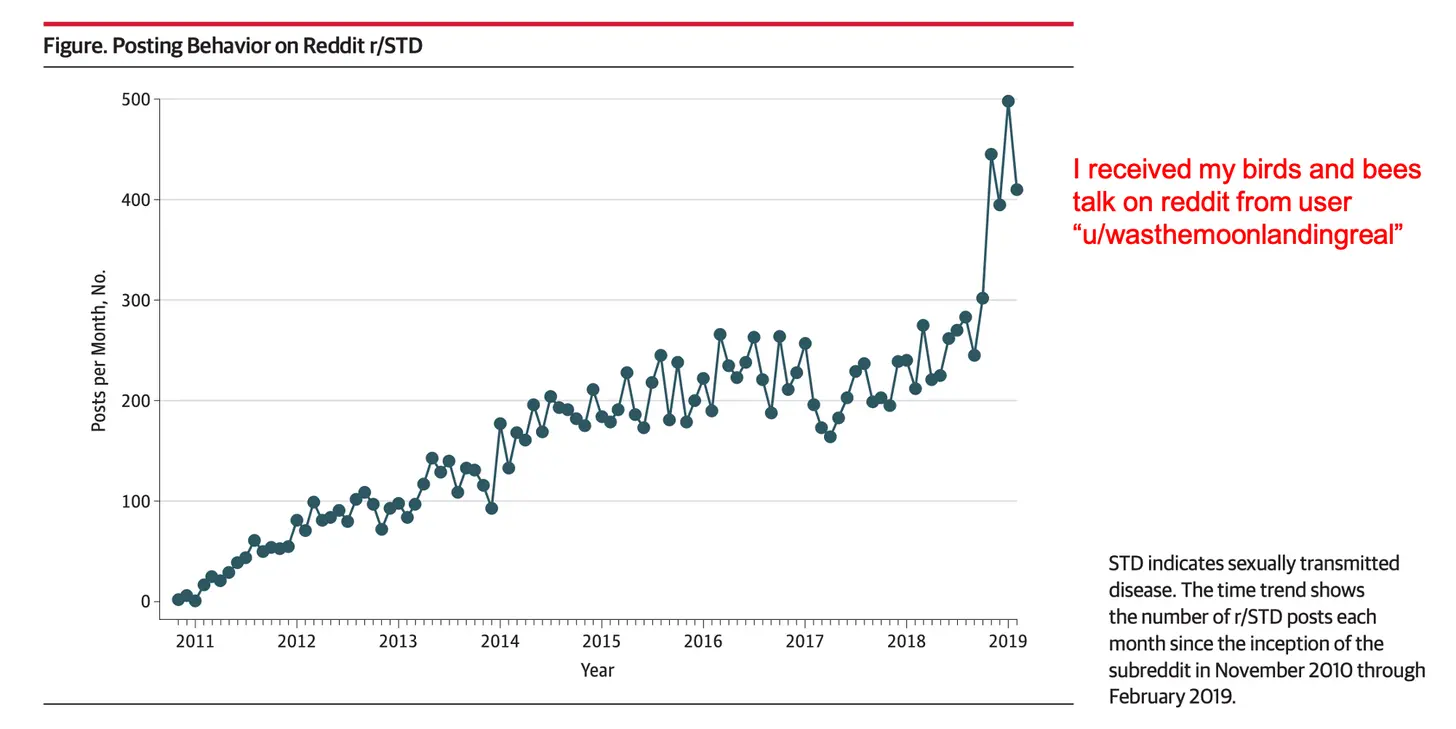
It’s not really that surprising then that most of the patient communities that have emerged around that time also followed a similar playbook - advertising. In fact the rates for advertising on a lot of these platforms were way higher than other social networks because the audience was much more targeted with way higher intent to actually use the products.
Some patient communities also realized that many of the members actually want their data to be used in research and will happily contribute to it. With patient consent these communities would send out sponsored surveys, sell de-identified data from aggregate patient profiles, and get patients' feedback or help with protocol design.

Candidly from people I’ve talked to, the data these patient community platforms capture directly is actually not very good and requires a lot of manual inputting on the patient’s side for things like medications you were on, diagnosis, hospitalization history, lab values, etc. Engagement is alright, especially with folks with unmet medical needs that life science companies are targeting. In this study, 1,323/7,000 PatientsLikeMe users with ALS, MS, and a few other diseases completed a survey sent to them (~19% completion). 19% may not sound like a lot but that’s actually pretty solid, especially when it comes to actually finishing relatively thorough surveys. That kind of engagement is how biopharma companies get the structured data they need that probably doesn’t just exist on the platform itself.
In this V1 business model there’s really only one main client - life sciences companies (or people that also sell to life sciences companies). The focus is on collecting data for that purpose and appealing to patients who have that intent. But after 10+ years there haven’t really been many exits. There was a fire sale exit for PatientsLikeMe and lots of smaller ones with companies that struggled to find a sustainable business model. Maybe this market isn’t that large or the right one to target.

{{interlude 4}}
Patient Communities V2 - Behavior changes, nudges, and payer/providers?
Outside of healthcare, social networks are evolving. New social networks create tools that then lead to communities (e.g. Discord using a voice chat tool to become a social network), creators are building their own communities around their content (like...me lmao), or exploring new mediums that blend online interactions with real life ones (e.g. Clubhouse hosting audio rooms you can pop into and listen in on). I think it makes sense that the next wave of patient social networks will similarly evolve and experiment.
Instead of just contributing data to new therapies, patient communities can actually modify patient behaviors as a result of the community through advice, reinforcement, and more. This feels like a use case that has way more opportunity to build for, and unlocks different business models that new players in healthcare would care about (specifically payers and providers). Plus it becomes appealing for patients that have conditions that are less sought after by biopharma companies.
PatientsLikeMe actually put out a paper looking at some of the things patients did because of the platform and a lot of it was lifestyle modifications, changing medications, and having more informed conversations with their physicians. Considering everyone is trying to figure out what their patient engagement strategy is, it’s hard not to think that patient communities would play an important part there.

New patient communities trying to elicit a behavior change and improve patient outcomes would have to be built from the ground up. They would need at the very least:
- More involved services (care delivery, moderators, etc.) and proactive involvement in the community instead of being just lurkers or mining data
- Specific outcomes that they can measure and track
- Products built for specific conditions vs. being disease agnostic like scales for tracking different biomarkers, integrations with wearables for that disease, tools to assist different lifestyle changes or functionality that the patient may have lost, etc.
- Also would help if they didn’t, you know, look like they were built in 2009
I posit that patient communities have to move beyond the traditional social network product of “we’re a platform for you to find others like you” and monetize attention. Instead they’ll use a combination of communities, digital tools, and services to actually help patients in their care journeys and get paid for outcomes or services rendered.
Insurance as a patient community? And other ideas
Three years ago I wrote a post about how insurance could be restructured into small pools. I...still don’t think this is a bad idea which means either I’ve stayed the same level of dumb or this is still undertapped.
The main premise is that insurance consists of pools of people that have different disease types, but insurance companies make no concerted effort to connect patients of similar disease types, despite all the research above that suggests patients care choices can actually be influenced by peers with a similar disease. Please ignore the childlike quality of my drawings.
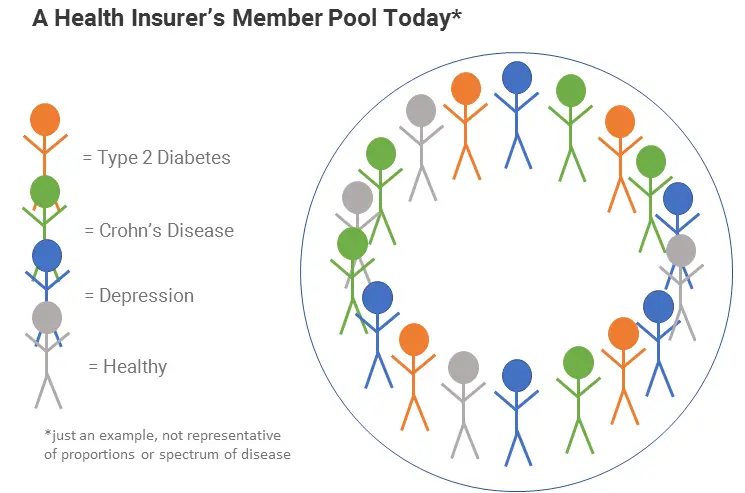
So my suggestion is that insurers actually help work with patient communities to make this happen because it’s financially lucrative to do so. My thought is:
- You sign up for a health insurer’s plan.
- You’re put into a group of 10 with people who have similar health profiles as you (age, family history, existing disease, etc.) and therefore relatively similar health goals. Identities would be anonymous by default, but opt-in to reveal more personal information.
- There are individual health goals given to you and then group goals for all 10 to reach. This would include primary care check ups, fitness goals, screenings, etc.
- A dual reward system exists for hitting personal goals and group goals. Many of the member-owned health plans emphasize the re-investment of their earnings back into the community — this could provide a tangible reinvestment avenue that’s theoretically transparent to members and a good marketing tool to get people interested.

Some health insurance plans like C-SNPs (Chronic Condition Special Needs Plans) already focus on the needs of specific patients within a given disease area (e.g. congestive heart failure). There’s probably benefits to connecting those patients within a plan.
UnitedHealth even ended up buying PatientsLikeMe, maybe reconfiguring the product to enable these patient to patient interactions would actually help patients (which would help UnitedHealth). I feel like Optum isn’t really that busy so maybe they should take on this project, too. 🙃
Some other ideas on the evolution of patient communities :
- Tools become communities - Doing a checklist of things required to do health maintenance is so boring. Why not make it a game with other people, which is de facto a community? For example Hinge Health has groups and leaderboards for things like plank challenges (lol I’m good). Gamify the steps and make them a community! Make Patient Reported Outcomes tools social! Use passive data collection as content for feeds (with patients choosing who can see it)! Measure the increase in outcomes for people doing those steps solo vs. with peer accountability!

- Group formats - I’ve tried personal trainers and I’ve tried group fitness classes, and both serve a purpose. The personal trainers give you one-on-one attention and help you build your personal routine, but the classes are social and way more energetic. Healthcare can be the same way, with your doctor being the “personal trainer” and group classes to supplement. I think group therapy, which companies like Pace and Coa have recently raised for, is an example of this. The concept of using groups isn’t new, but virtualizing it means that you can do it with people that don’t live anywhere near you (which could be important for stigmatized issues like AA).
Or on the flipside, maybe it makes certain healthcare activities, dare I say, fun? Maybe healthcare doesn’t need to be super sensitive, and for certain maintenance things like physical therapy, it could be fun to bring a friend that’s also doing the same maintenance activities.
- Doctors as moderators - If doctors are seeing patients with similar issues, wouldn’t it make sense for them to connect patients within their patient panel (assuming they’re open to it)? What if doctors, nurse practitioners, occupational therapists, etc. became moderators in micro patient communities they ran? It would be a good way to stay engaged with patients outside of the clinic and might even attract new patients who want to be a part of this community or found the doctor through it.
Conclusion
There’s a lot more to be said about patient communities, so part 2 will talk about some feature considerations when building a community and a few investments I’ve made that are actually built on some of these ideas.
I think we’re in the very early innings of “social healthcare”, and new patient communities will be a key part of that movement.
Thinkboi out,
Nikhil aka. “PatientsLikeYouToo don’t worry”
Twitter: @nikillinit
Quick interlude - Healthcare 101! Upcoming conferences!
See All Courses →A few quick things - Healthcare 101 starts soon! Let me teach you how healthcare works, cause this mess is confusing.
If you need to look smart in front of healthcare clients, get your team up to speed quickly on how healthcare works, or you’re trying out where in healthcare you want to build…this course is for you.

Also…we have 3 big events coming up.
- Healthcare Data Camp for anyone who touches healthcare data
- A new healthcare software engineering conference in New York on 9/18 (opening soon)
- Ops Knowledgefest, for healthcare ops people in SF on 10/17 (opening soon)
We’re going to launch all of these things very soon so keep an eye out. If these are areas you want to know sponsorship options, we should chat.
Quick Interlude - Data Camp Applications Due Soon!!
See All Courses →Don’t forget…DATA CAMP IS COMING TO YOU THIS JUNE! Applications are due 4/24, but fill it out now before you forget. More details on the site. It’s all breakouts, a small curated group, and focused on tactical things to bring to work on Monday.
We’re also taking our first sponsors now - so if you want to get in front of data engineers/healthcare data pros, let us know.

Quick Interlude - Data Camp Applications Due Soon!!
See All Courses →Don’t forget…DATA CAMP IS COMING TO YOU THIS JUNE! Applications are due 4/24, but fill it out now before you forget. More details on the site. It’s all breakouts, a small curated group, and focused on tactical things to bring to work on Monday.
We’re also taking our first sponsors now - so if you want to get in front of data engineers/healthcare data pros, let us know.








