How Much Info Should A Patient Get?
Get Out-Of-Pocket in your email
Looking to hire the best talent in healthcare? Check out the OOP Talent Collective - where vetted candidates are looking for their next gig. Learn more here or check it out yourself.
 Hire from the Out-Of-Pocket talent collective
Hire from the Out-Of-Pocket talent collectiveAI x RCM Masterclass
.gif)
Healthcare 101 Crash Course
%2520(1).gif)
Featured Jobs
Finance Associate - Spark Advisors
- Spark Advisors helps seniors enroll in Medicare and understand their benefits by monitoring coverage, figuring out the right benefits, and deal with insurance issues. They're hiring a finance associate.
- firsthand is building technology and services to dramatically change the lives of those with serious mental illness who have fallen through the gaps in the safety net. They are hiring a data engineer to build first of its kind infrastructure to empower their peer-led care team.
- J2 Health brings together best in class data and purpose built software to enable healthcare organizations to optimize provider network performance. They're hiring a data scientist.
Looking for a job in health tech? Check out the other awesome healthcare jobs on the job board + give your preferences to get alerted to new postings.
Today I want to ask a new discussion question for you to chew on over the long weekend.
To reiterate the rules:
I’ll pose a question and give my thoughts if I have any, and in a future newsletter include ~3 of my favorite answers people reply with. I’ll possibly even make a meme related to your answer.
Good answers are ones with a novel viewpoint, data to back up their claim, personal stories, and avoid clearly shilling something.
Please reply to this email with your thoughts on the question and let me know if you want to have your name or be anonymous. You have to actually be on the newsletter to submit a reply to it obviously.
Try to keep answers to 2 paragraphs or less please. This obviously doesn’t apply to me because it’s my newsletter and these are house rules.
--
Question: How much data should be available to patients in their medical record? Specifically should patients be able to see their lab results as soon as they come and the doctor’s notes about them.
I saw this tweet making the rounds the other day and it generated a lot of discussion in some of my healthcare circles (as if I have others).
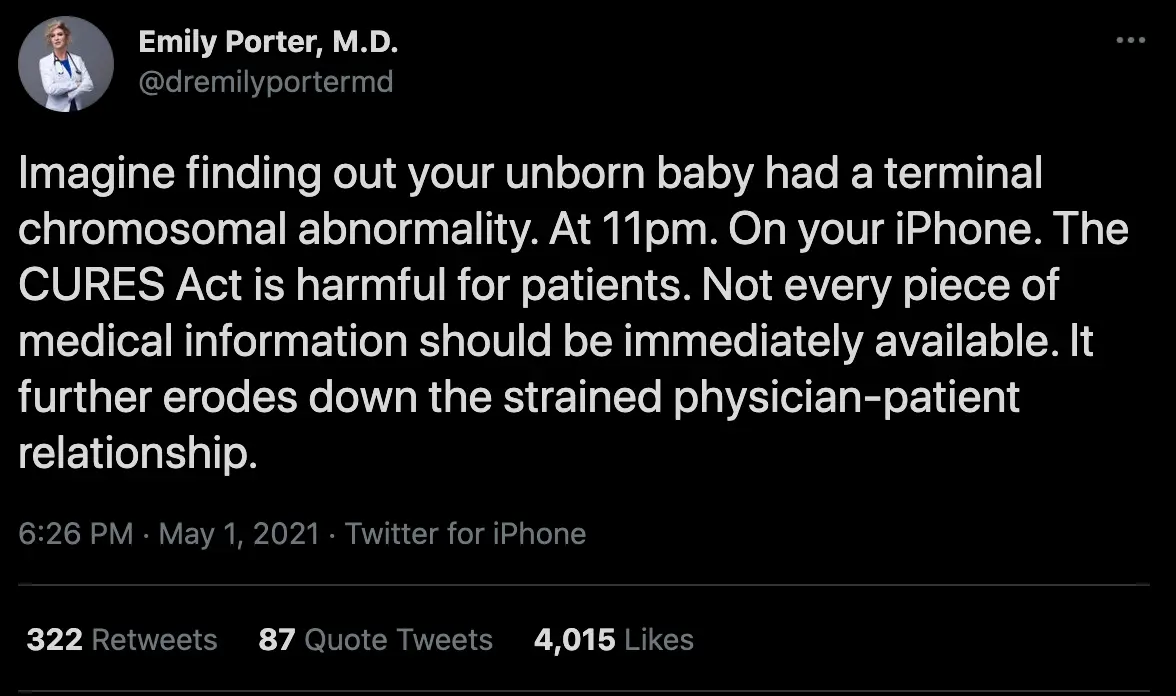
In general healthcare is trending towards giving patients more information, faster. Patients will be notified of a lab result before and look at it without a physician explaining the results to them.
There’s also new information now being made available to patients. For example, thanks to the 21st Century Cures Act and Anti-Information Blocking Rules, these sets of clinical notes are now accessible to a patient.
- Consultation notes
- Discharge summary notes
- History & physical
- Imaging narratives
- Laboratory report narratives
- Pathology report narratives
- Procedure notes
- Progress notes
The thing is that a lot of these notes are in patient files but have historically been meant for other clinicians. Sometimes they’ll say things like “patient is irritable” or will use clinical definitions like “morbidly obese” which maps to an ICD-10 code for reimbursement purposes. If a patient reads this, they could be understandably offended.
One camp will say that this is information that can be misinterpreted easily or includes things patients don’t need to know. It can cause patients to take very drastic measures if they misunderstand a result, or create unnecessary friction with the physician if they see information the physician has written about them that they disagree with.
It probably won’t come as a shock to you that I think patients should have the option to get this data immediately, and should be able to choose if they want to hear it from a physician or not. The onus is on the medical system to be better at giving patients information alongside these notes and lab results that can explain what they mean in terms they can understand.
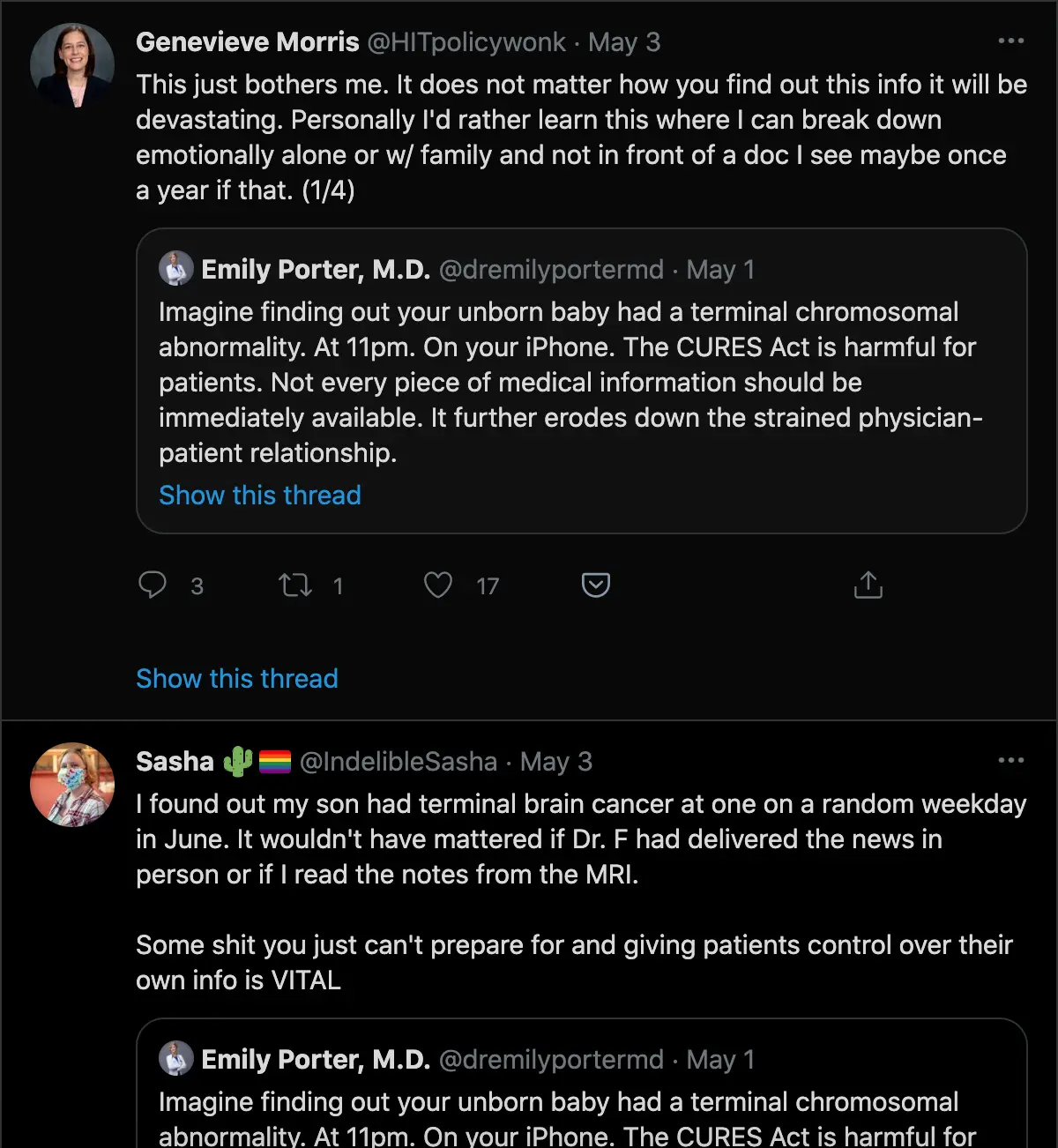
IMO a big reason people distrust the healthcare system is because of the level of paternalism that patients face and the belief that they can’t handle this information. Actually if you scroll through the quote tweets of the initial lab result tweet, you can see a ton of patients disagree strongly with this take with their own stories about being extremely anxiety ridden waiting for the results or having a terrible experience being told by a physician.
I do worry that on the notes side, physicians will just end up moving a lot of the “uncomfortable” parts of the note into texts/whatsapps with physicians they work with instead of writing it on the note itself. This is bad because those are still important parts of the record and would no longer travel with the full patient record if they moved around. I also can just imagine how much the machine learning models are going to break if the physicians end up changing how they write notes to change clinical terms into ones patient’s can understand.
What do you think? Will patients be able to handle this information, or is this a bad thing?
Thinkboi out,
Nikhil aka. "you want the data? YOU CAN'T HANDLE THE DATA"
Twitter: @nikillinit
Quick interlude - Healthcare 101! Upcoming conferences!
See All Courses →A few quick things - Healthcare 101 starts soon! Let me teach you how healthcare works, cause this mess is confusing.
If you need to look smart in front of healthcare clients, get your team up to speed quickly on how healthcare works, or you’re trying out where in healthcare you want to build…this course is for you.

Also…we have 3 big events coming up.
- Healthcare Data Camp for anyone who touches healthcare data
- A new healthcare software engineering conference in New York on 9/18 (opening soon)
- Ops Knowledgefest, for healthcare ops people in SF on 10/17 (opening soon)
We’re going to launch all of these things very soon so keep an eye out. If these are areas you want to know sponsorship options, we should chat.
Quick Interlude - Data Camp Applications Due Soon!!
See All Courses →Don’t forget…DATA CAMP IS COMING TO YOU THIS JUNE! Applications are due 4/24, but fill it out now before you forget. More details on the site. It’s all breakouts, a small curated group, and focused on tactical things to bring to work on Monday.
We’re also taking our first sponsors now - so if you want to get in front of data engineers/healthcare data pros, let us know.

Quick Interlude - Data Camp Applications Due Soon!!
See All Courses →Don’t forget…DATA CAMP IS COMING TO YOU THIS JUNE! Applications are due 4/24, but fill it out now before you forget. More details on the site. It’s all breakouts, a small curated group, and focused on tactical things to bring to work on Monday.
We’re also taking our first sponsors now - so if you want to get in front of data engineers/healthcare data pros, let us know.








