What's The Deal With Telemedicine?
Get Out-Of-Pocket in your email
Looking to hire the best talent in healthcare? Check out the OOP Talent Collective - where vetted candidates are looking for their next gig. Learn more here or check it out yourself.
 Hire from the Out-Of-Pocket talent collective
Hire from the Out-Of-Pocket talent collectiveHealthcare 101 Crash Course
%2520(1).gif)
Featured Jobs
Finance Associate - Spark Advisors
- Spark Advisors helps seniors enroll in Medicare and understand their benefits by monitoring coverage, figuring out the right benefits, and deal with insurance issues. They're hiring a finance associate.
- firsthand is building technology and services to dramatically change the lives of those with serious mental illness who have fallen through the gaps in the safety net. They are hiring a data engineer to build first of its kind infrastructure to empower their peer-led care team.
- J2 Health brings together best in class data and purpose built software to enable healthcare organizations to optimize provider network performance. They're hiring a data scientist.
Looking for a job in health tech? Check out the other awesome healthcare jobs on the job board + give your preferences to get alerted to new postings.
Today I have a new post and discussion topic.
To reiterate the rules:
I’ll pose a question and give my thoughts. In a future newsletter I’ll include ~3 of my favorite answers people reply with. I’ll possibly even make a meme related to your answer.
Good answers are ones with a novel viewpoint, data to back up their claim, personal stories, and avoid clearly shilling something.
Please reply to this email with your thoughts on the question and let me know if you want to have your name included or be anonymous. You have to actually be on the newsletter to submit a reply to it obviously.
Try to keep answers to two paragraphs or less please. This obviously doesn’t apply to me because it’s my newsletter and these are house rules.
What's Happening In Telemedicine Today? What Could Be Improved And What's Stopping Adoption?
During COVID, conversations around telemedicine hit the top spot in healthcare, displacing “personalized medicine” and the phrase “you can’t move fast and break things in this industry”.
I made a little bingo board so you can stay entertained through your next conversation about telemedicine. These were just some of the most common tropes that came to mind.
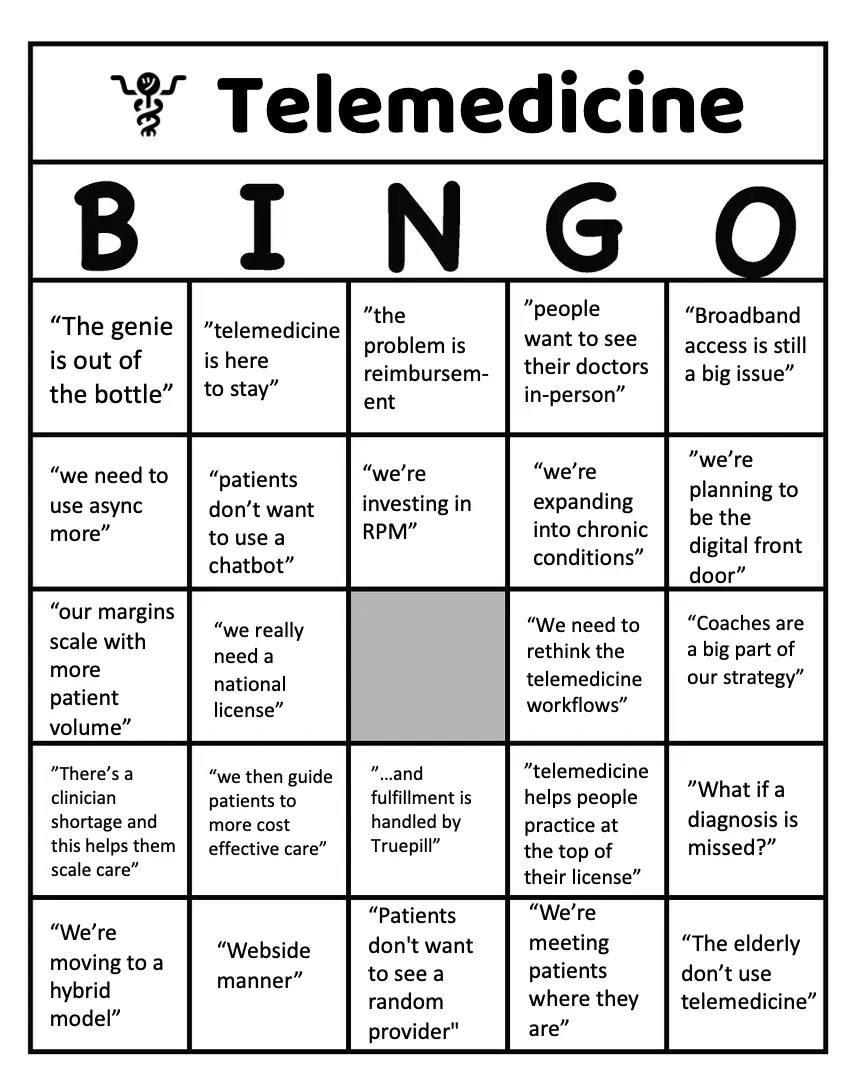

I want to hear some of your thoughts on where you think telemedicine is going. Let’s level set with some context.
Telemedicine moves back to the future
Prior to COVID, telemedicine was a very small percentage of visits. Then, during COVID, it spiked to more than 75% of visits, and now it seems to have leveled out. But it’s still considerably above pre-COVID levels; Mckinsey estimates it’s about 38x above 2019 levels and ~30-40M telemedicine claims are filed per month. Fair Health pegs it at ~4.5% of medical claims vs. a peak of 13% at the height of COVID + there is a clear discrepancy based on specialty. A lot of these telemedicine analyses have their own flaws because they rely on claims and CPT codes which will skew based on payer type and won’t include many types of transactions (e.g. cash pay, non-billable messaging, waived co-pays, etc.), so all of it should be taken with a grain of salt.
On top of that, more reimbursement codes for remote patient monitoring and remote therapeutic monitoring (aka. medical hardware that monitors patient vitals + give guidance on what to do) has made it more financially viable to include home monitoring as a part of telemedicine care.

But now, as we ease back into normalcy, the future of telemedicine is a bit up in the air. In fact, it seems like the system is using telemedicine but trying as hard as possible to retrofit to the existing system - giving the worst of both worlds by increasing the amount of healthcare consumption and prices.
- Hospitals are getting wonky with charges. Some are deciding whether a MyChart message counts as a separate billable message. This gets complicated because if the message is “technically” billable and you offer it for free, it can look like inducement if you DON’T bill for it. Anecdotally, I’ve heard that Epic has grown from 10k messages/month to 2.5M /month. Others have even started charging facility fees for patients based on…where the doctor is taking the telemedicine visit? And they’re justifying it based on…what now? I’m going to assume this entire dialogue is satire.
“She called the billing office the next morning and was told the facility fee is based on where the doctor is located. Since the doctor would be on hospital property, the hospital would charge a facility fee of between $50 and $350, depending on her insurance coverage…”
”’It offsets the cost of the software we use to facilitate the telehealth visits, and we do still have to keep the lights on,’ he said, noting that the providers doing telehealth visits are on hospital sites that incur heat and power and maintenance charges.”
Bruh.
- Telemedicine still seems to mostly happen as either a phone call or video visit, which is essentially the same as an in-person visit in terms of efficiency (sometimes even worse, think about all the technical issues with Zoom calls). If physicians or aggregate care teams can’t see way more patients in a day, then the costs are the same and we haven’t improved care accessibility in the dimensions that matter. Blended models and asynchronous telemedicine are still not the norm.

- CPT codes are a set of codes we use to reimburse healthcare services that are designed to either measure the complexity or time that goes into a given service. However, this underpinning philosophy and process means that there’s no incentive to make services rendered more efficient. For example, some CPT codes have time requirements, defeating the purpose of having more efficient visits via telemedicine. (CPT code 98980 requires a 20 minute interactive visit for remote patient monitoring services and then CPT code 98981 gives more for an additional 20 spent.) If billing is set up around time minimums with a person, how are you supposed to build efficient or fully automatic systems? Plus, relying on CPT codes also makes it hard to give cost estimates/guarantees to patients up front.
- Payment parity rules (aka. the reimbursement for a virtual and in-person visit needs to be the same) are great for providers who probably wouldn’t invest in telemedicine otherwise, but bad for anyone that wants to give incentives for patients to see virtual providers instead. Plus the extra money that ends up going to providers still comes from patients, just more indirectly in the form of premiums, taxes, etc.
- McKinsey recently put out these survey results suggesting that while telemedicine is something patients seem to want more of, physicians are not huge fans and also haven’t really invested in it. It’s amazing to me that providers and physicians will complain about patient engagement when they don’t want to meet patients where the patient wants to be met.

Right now, telemedicine is in its awkward teenage years - uncomfortably in-between trying to fit onto an existing care delivery system that wasn’t built to use it but without a clear system of reimbursement for companies that want to use it natively. Compared to my teenage years, less Sum 41 is involved but somehow there’s more fixation on erections?
{{interlude 4}}
The telemedicine conundrum
Some of my disjointed thoughts:
- Telemedicine 1.0 almost exclusively focused on one-off patient transactions (urgent care, ecommerce style product shopping, face-to-face visit with your doc for a follow-up) and that’s also reflected in the data. This means they built products that are optimized to bill for that transaction and are not really built for longitudinal care. Most of them are either just replicating a face-to-face visit online, or using one-time forms with an anonymous doc. This is why I think a lot of the companies that are trying to shift from one-time relationships to longitudinal ones (become your PCP, chronic care management, etc.) are struggling to make that shift because their products weren’t actually built for that and it’s not how consumers think about a lot of these brands.

- Telemedicine companies purpose-built for value-based care contracts look very different. They have to build care teams, hire admin teams that are trained in telemedicine, heavily use asynchronous chat, figure out the handoffs between clinical vs. non-clinical teams, use some sort of risk-stratification system to understand when to intervene proactively, have some sort of e-specialist and referral network to triage patients appropriately, and develop offline care strategies (both sending the right level of care to someone’s home or networks of in-person locations to send someone). In fact, they probably won’t be called “telemedicine” companies at all because they’ll be hybrid, with some that skew to more in-person for complex populations. A new wave of companies are building virtual-first health plans in every health insurance segment: Galileo + MVP Healthcare in Medicaid, Cigna and MDLive in commercial, Firefly for small/midsize employers, Alignment Healthcare’s virtual HMO in Medicare Advantage, and I’m sure there are more I’m forgetting.
- Telemedicine 1.0 was mostly designed to give patients a smooth experience, but cared less about physician tooling or experience. Plus for large health systems, the buyer was hospital admin vs. the physician users which also led to less than desirable physician tools and workflows. Many physicians have to shoehorn telemedicine-specific visits into their workdays of in-person visits and go through totally separate rooms/processes/tools to do them. And these reasons are why physicians aren’t huge fans of telemedicine IMO. New telemedicine companies not only need to invest in better tooling if they’re caring for patients with more complex conditions, but it’s also become a form of clinician retention now that the market for clinicians is so hot. It can actually be a way to recruit talent. In tandem, there are tools built to make the infrastructure for that tooling better, e.g. Canvas, which has built an EMR that’s way more flexible and programmable for virtual care.

- I have yet to see a paper that talks about the number of missed diagnoses during a telemedicine visit compared to the number of missed diagnoses during a face-to-face visit. This seems to be a common talking point amongst physicians, but is there data to back the claim up that telemedicine will miss things? Genuine question.
- Telemedicine is going to be where large health systems get caught flat footed vs. startups. Hospitals have massive physical footprints with every incentive to bring patients through their doors or use the sus billing maneuvers to make money during telemedicine visits. In fact, payers SHOULD lean much more into reimbursing new telemedicine first companies in some value-based arrangement because it's theoretically in their best interest. However, I’m told that most telemedicine companies still try to negotiate individual case rates vs. trying to create any longer term ROI guarantee. Some of the virtual-first health plan partnerships I listed above are a start, but I think we’ll see more here.
- I’m interested to see how more telemedicine companies lean into the inclusion of peers + online groups as part of their programs. Most telemedicine companies I’ve seen are one-to-one between patient and provider/care team. I still think using opt-in for peer support, leaderboards, tracking, private Yelp for assessing in-person care, etc. would be a good way for patients to learn from others like them in combination with a clinician. WellTheory is doing some of this in autoimmune care, Groups does some of this in addiction treatment, and I’ve seen a few others in different types of obesity management telemedicine companies.

In general, I see telemedicine as a feature of new care delivery companies and necessary for new workflows, but not necessarily a standalone business. We’re already shifting away from the telemedicine businesses that aims to virtualize the inefficient in-person experience. I think our fixation on the number of billable telemedicine visits that have occurred is the wrong way to look at this. Telemedicine used correctly helps enable a better longitudinal patient relationship and better product/user experience that encounter-based billing will never be able to capture.
Tell me your hottest takes on telemedicine. Will it get adopted more broadly or will it never be a thing? What’s stopping it from getting adopted today? Is it good or bad for society? What do you think about the current state of telemedicine affairs?
Thinkboi out,
Nikhil aka. “Sending my doc funny TikToks on MyChart”
Twitter: @nikillinit
Other posts: outofpocket.health/posts
Thanks to Sahir Jaggi, Alex Bertha, and Morgan Cheatham for looking at drafts of this.
{{sub-form}}
---
If you’re enjoying the newsletter, do me a solid and shoot this over to a friend or healthcare slack channel and tell them to sign up. The line between unemployment and founder of a startup is traction and whether your parents believe you have a job.
But first…DATA CAMP APPLICATIONS CLOSE SOON
See All Courses →If you’re into healthcare data and want to be around other healthcare data nerds, you really should apply to Data Camp ASAP!! The people are saying nice things about it because we do a lot of really awesome workshops to make you better with healthcare data.
Applications are due 4/24, BUT YOU WILL FORGET SO DO IT NOW IT TAKES LIKE 5 MIN IF YOU’RE SMART.
And sponsors…we’re already talking to people and have a limited number of slots. Hit me up if you want to see the packet.
And if you’re REALLY a healthcare data nerd…you’ll want to come to our AI x Risk Adjustment FREEEEE course. You’ll learn at least a thing or two, and probably a lot more. Starts 4/22 (aka…right before data camp applications!)

Quick Interlude - Data Camp Applications Due Soon!!
See All Courses →Don’t forget…DATA CAMP IS COMING TO YOU THIS JUNE! Applications are due 4/24, but fill it out now before you forget.
More details on the site. It’s all breakouts, a small curated group, and focused on tactical things to bring to work on Monday.
We’re also taking our first sponsors now - so if you want to get in front of data engineers/healthcare data pros, let us know.

Quick Interlude - Data Camp Applications Due Soon!!
See All Courses →Don’t forget…DATA CAMP IS COMING TO YOU THIS JUNE! Applications are due 4/24, but fill it out now before you forget. More details on the site. It’s all breakouts, a small curated group, and focused on tactical things to bring to work on Monday.
We’re also taking our first sponsors now - so if you want to get in front of data engineers/healthcare data pros, let us know.








